Dentistry in England changed beyond recognition on the 25th March 2020. In the middle of the morning, every dentist in the country received a letter via email from the Chief Dental Officer (CDO) telling us to down tools and cease seeing patients face-to-face. It followed similar letters from the CDOs of the other nations of the union to their respective practitioners. Although the CDO technically only holds sway over NHS practice, the majority of private practices also stopped seeing patients.
By the end of the day, routine dentistry across the UK had ground to a halt with no idea of when it would resume. If you had a dire emergency, you could be referred to an Urgent Dental Centre (UDC) which were hurriedly set up by the NHS to provide care for those who had ongoing pain. But the scope of treatment in UDCs was initially limited, often only being able to remove teeth. Understandably, the shutdown of routine dental practice has had a deleterious effect on the dental health of the nation. The cause? As with most things in 2020, COVID-19.
As you read this, many practices are back open, able to see patients. The UDC system is still running, but with an expanded scope for treatment. But what are the risks of going to the dentist at the moment? What are dentists doing about those risks? And, most importantly, is it safe?
Let’s start with some basics. As SARS-CoV-2, the virus which causes COVID-19, has been studied, we’ve learned more about its mode of transmission. Initially, many believed that surface to surface contact was the primary method of spread, but it’s now thought that respiratory aerosols are the key route. For dentists, this, theoretically at least, causes a problem.
Dentists are quite literally in the firing line when it comes to respiratory aerosols. You lot breathe, cough and sneeze on us every single day of our practicing lives.
Dentists are quite literally in the firing line when it comes to respiratory aerosols. You lot breathe, cough and sneeze on us every single day of our practicing lives. And many of the tools we use to do our job produce significant amounts of aerosols themselves. The handpieces (drills) and ultrasonic instruments (such as the scalers that your dentist or hygienist regularly use) all spray out a fine mist of aerosol that not only mixes with your saliva but can cause it to be aerosolised itself into the atmosphere of the dental surgery.
It’s perhaps understandable then that given the theoretical risks of treatment we had to stop seeing patients face to face. But now we’re back, so what’s changed?
Well, firstly, we know more about the virus. It may sound obvious, but at the beginning of the pandemic, the precautionary principle had to apply, purely due to the number of unknown factors concerning SARS-CoV-2 and the spread of COVID-19. Work done by several groups over the first period of lockdown allowed for the production of guidelines for safe practice. Each practice should by now have constructed their own Standard Operating Procedure (SOP) drawing on these guidelines, and tailor-making them to their practice. This document should give clear guidance to everyone in the practice on how to best care for patients in a safe way, from new cleaning routines to ensuring minimal contact time between everyone in the building. Most importantly, it will include many factors to ensure that any treatment provided is as safe as possible.
Talking of treatment, the way that dentists classify the treatment we provide has changed. Before COVID, no matter what you were turning up to have done, my appointments would have always had roughly the same structure: Say hello to the patient, have a chat about what we were going to do, make sure my hands were clean, pop some gloves and a surgical mask on, do whatever needs doing then say goodbye to the patient. Pretty simple.
In a post-COVID world, everything is now either an Aerosol Generating Procedure (AGP) or a Non-Aerosol Generating Procedure (Non-AGP). You can probably guess what the difference is. Procedures classed as AGPs generally include most fillings, root canal treatment and the use of an ultrasonic scaler for example. Non-AGPs include examinations (that’s check-ups to most people), straightforward extractions and the various stages of making dentures.
If you’re coming in for a non-AGP appointment, the only real difference you’ll see in the surgery is that I’ll be wearing a disposable apron and I’ll have a surgical mask on at all times. When I look in your mouth, I’ll have a visor on as well. Dental surgeries generally have high levels of infection control, with strict procedures to follow after every patient. For low-risk procedures, even during the COVID-19 pandemic, these standard precautions are adequate to ensure patient and practitioner safety.

With AGPs, it’s a different ball game. Firstly, dentists and their nurses have to wear enhanced PPE. This means some form of surgical gown and a high filtration mask. These are a bit cumbersome and reduce the ability to communicate, but otherwise, I’ve found them to be generally OK. Many others have not, with some of the masks being uncomfortable when used for extended periods.
The real issue is that once we’ve done treatment, we have to vacate the room and leave the aerosol to settle before someone can clean it. For many surgeries, this is a significant problem. If you work in a small practice, this could leave you with swathes of downtime where you can’t access your surgery to see patients. Initially, this fallow time, as it’s called, was an hour. More recently, thanks to work by the people of the Scottish Dental Clinical Effectiveness Programme amongst others, we’ve been able to adopt a more granular approach, reducing fallow times to as little as 10 minutes in some circumstances. This has enabled routine dentistry to return in many practices, but in many others, there are still issues to overcome, which is delaying their return to regular care.
There are still questions about how risky AGPs are. It may be that we’re being overcautious with our guidelines. If we stop to think for a minute about the aerosols produced in a dental setting, there are a variety of sources. Obviously, dentist, nurse and patient will be producing respiratory aerosols just by breathing. But our current guidelines suggest that face coverings and maintaining social distancing as much as possible mitigate against that, so the aerosols we’re attempting to protect ourselves from during AGP appointments are of a dental origin. They come from our handpieces and ultrasonic units. And they’re not respiratory aerosols. They’re clean water, that’s treated with a disinfectant. This clearly isn’t going to increase the risk of COVID transmission, although if it mixes with saliva and this saliva is projected into the air, then there is an escalation of risk. But guess what? That straw like device that nurses use to stop you from drowning while you’re having a filling also sucks up potentially COVID containing aerosols.
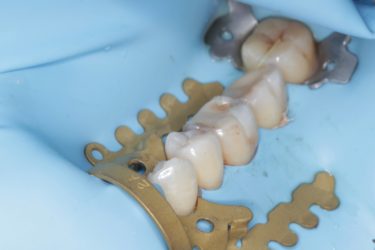
Also, if we use a rubber dam, a sheet of material that we punch holes in to isolate your teeth from the rest of your mouth, the amount of our clean water mixing with your unclean saliva is reduced to virtually nothing. It’s quite possible that actual treatment is much less of a risk than we’re assuming it is. But the evidence isn’t there. So again, we must act with an abundance of caution.
So, back to the original question of how safe is it to go to the dentist at the moment? Pretty safe, actually. The dental profession has an already high standard of infection control protocols. In addition to this, we’ve taken all kinds of extra measures to protect you, us and the outside world. And, as far as I’m aware, there have been no recorded cases of COVID transmission from dental appointments. Having said that, low risk doesn’t mean no risk. Coming to see us is riskier than staying at home, but probably not as risky as going to the pub or supermarket. You might want to consider delaying your appointment if it’s not super urgent, or if you’re in a higher risk group. But we’re here to help you if you need us.



