Several US doctors, including the guru of all things alternative, Andrew Weil, recently published a paper (Integrative medicine considerations for convalescence from mild-to-moderate COVID-19 disease (nih.gov)) in which they offered a definition of Integrative Medicine (IM) that I had not yet come across:
Integrative medicine is defined as healing-oriented medicine that takes account of the whole person, including all aspects of lifestyle. It emphasizes the therapeutic relationship between practitioner and patient, is informed by evidence, and makes use of all appropriate therapies.
Ever since the term IM became fashionable – here in Britain it was Prince Charles, the indefatigable pioneer of quackery, who really popularised ‘Integrated Medicine’ – there have been dozens of definitions of the term. It is almost as though IM proponents are not quite sure themselves what it is that they are promoting. And ever since I first heard about IM, I felt it was a thinly disguised attempt to smuggle unproven treatments into the routine of evidence-based medicine (EBM).
In 2002, I published my 1st comment on the subject. In it, I cautioned that IM must not become an excuse for using every conceivable untested treatment under the banner of holism. Nineteen years on, this is exactly what has happened, and one definition of IM after the next seems soaked in platitudes, falsehoods and misunderstandings.
So, let’s see how reasonable this new definition is. I will try to do this by briefly discussing each of its elements.
IM is healing-oriented medicine
I must admit, this made me laugh when I first read it. Does anyone know a medicine that is not oriented towards healing? After all, healing is defined as the process of becoming well again, especially after a cut or other injury, or of making someone well again. Healing is what medicine has always been and always will be about. In other words, it is not something that differentiates IM from other forms of healthcare.
IM takes account of the whole person
This is the little holistic gimmick that IM proponents like to adopt. It implies that normal healthcare or evidence-based medicine (EBM) is not holistic. The implication is, however, demonstrably wrong. Any good medicine is holistic, and if a sector of healthcare fails to account for the whole person (which, of course happens), we need to reform it.
Here are the conclusions of an editorial on this subject I published in 2007 entitled ‘Holistic heath care?‘:
good health care is likely to be holistic but holistic health care, as it is marketed at present, is not necessarily good. The term ‘holistic’ may even be a ‘red herring’ which misleads patients. What matters most is whether or not any given approach optimally benefits the patient. This goal is best achieved with effective and safe interventions administered humanely — regardless of what label we put on them.
Creating a branch of medicine that, like IM, pretends to have a monopoly on holism can only hinder this process.
IM includes all aspects of lifestyle
Really, all of them? This must be nonsense! Good physicians take into account the RELEVANT lifestyles of their patients. If, for instance, my patient with intermittent claudication is a postman, his condition would affect him differently than a patient who is a secretary. But ALL lifestyles? No! I fear this ‘over the top’ statement merely indicates that those who have conceived it have difficulties differentiating the important from the trivial.
IM emphasizes the therapeutic relationship
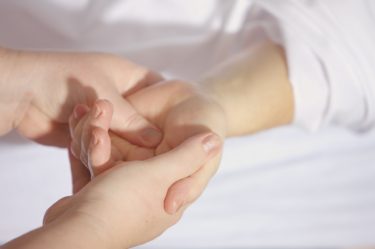
That’s nice… but so do all other physicians (except perhaps pathologists). As medical students, we were taught how to do it, some physicians wrote books about it (remember Balint?), and many of us ran courses on the subject. Some conventional clinicians might even feel insulted by the implication that they do not emphasise the therapeutic relationship.
Again, the IM brigade take an essential element of good healthcare as their monopoly. It almost seems to be an unpleasant habit of theirs to highjack a core element of healthcare and declare it as their very own invention.
IM is informed by evidence
Finally there emerges a real and fundamental difference between IM and EBM! While proper medicine is BASED on evidence, IM is merely INFORMED by it. The difference is stark, because it allows IM clinicians to use any un- or disproven treatment, no matter whether it is based on evidence or not. The evidence for homeopathy fails to show that it is effective? Never mind, IM is not evidence-based, it is evidence-informed. IM physicians know homeopathy is a placebo therapy (if they didn’t, they would be ill-informed which would make them unethical), but they nevertheless use homeopathy (try to find an IM clinic that does not offer homeopathy), because IM is not EBM. IM is evidence-informed (EIM)!
IM makes use of all appropriate therapies
This last element of the new definition takes the biscuit. Are the IM enthusiasts honestly suggesting that conventional doctors use inappropriate therapies? Does anyone know a branch of health care where clinicians systematically employ therapies that are not appropriate? Appropriate means suitable or right for a particular situation or occasion. Are IM practitioners the only ones who use therapies that are suitable for a particular situation?
I fear that this analysis confirms yet again that IM is little more than a smokescreen behind which IM advocates try to smuggle SCAM into routine healthcare. The fact that, during the last two decades, its definition constantly changed, while no half-decent definition has emerged suggests that the IM enthusiasts themselves don’t quite know what it is. My advice to them therefore is to adopt what Mark Crislip stated about IM:
“If you integrate fantasy with reality, you do not instantiate reality. If you mix cow pie with apple pie, it does not make the cow pie taste better; it makes the apple pie worse.”



